Op-ed: Semaglutide and the Algorithmic Border of Global Health
This photo provided by Eli Lilly in April 2026 shows manufacturing of the company's weight loss pill, Foundayo, at a plant in Carolina, Puerto Rico. (Eli Lilly via AP)
A new class of weight-loss drugs is quietly redrawing the boundaries of global health. Originally developed for diabetes, medications built on the semaglutide molecule have rapidly become among the most sought-after treatments for obesity, offering sustained metabolic effects that have repositioned these drugs at the center of pharmaceutical demand. What was once a specialized therapy, has evolved into a focal point of tension between global need and the institutional structures that govern access.
This shift is now reaching a crucial moment. In India, the semaglutide patent is set to expire, allowing local manufacturers to produce their own generic versions. This change is expected to drive prices down, and open up access for millions of people. What has so far been an expensive injection, mostly limited to wealthier patients, is now on the verge of becoming widely available as competition increases and production ramps up.
India’s role in this shift reflects its long-standing identity as the “pharmacy of the world,” a reputation built on turning expensive breakthroughs into affordable, mass-market medicines. Its drugmakers supply around 40% of the generic medicines used in the United States, making India a key player in expanding access to healthcare. In this light, semaglutide is more than just another product moving through its life cycle: it has become a test case for “metabolic sovereignty,” revealing how a country’s manufacturing capacity can redefine who ultimately gains access to treatment.
At the same time, the scientific landscape surrounding health is becoming increasingly fragmented. Public discourse reflects a growing divide not only between institutional standards and individual skepticism, but between competing claims about what constitutes credible evidence. In the midst of the current weight-loss craze, a growing movement of influencers encourages audiences to question what they are told, directly challenging the authority of the medical establishment. In this environment, influencers increasingly reframe substances, like nicotine, as “natural” wellness tools, promoting them for cognitive and neurological benefits despite evidence that remains preliminary and far from definitive.
Public discourse, however, does not apply this skepticism evenly. Some conversations downplay specific risks, while others subject them to careful scientific review. Recent studies suggest that GLP-1 drugs may help reduce addiction by acting on the brain’s reward pathways, directly pushing back against narratives that frame substances like nicotine as beneficial. At the same time, regulatory views continue to shift: the FDA recently reported “no increased” risk of suicidal thoughts linked to these drugs, revising earlier assessments that had left the question open. Taken together, these developments highlight a landscape in which competing readings of the evidence shape how we understand risk and, ultimately, which treatments the public deems legitimate.
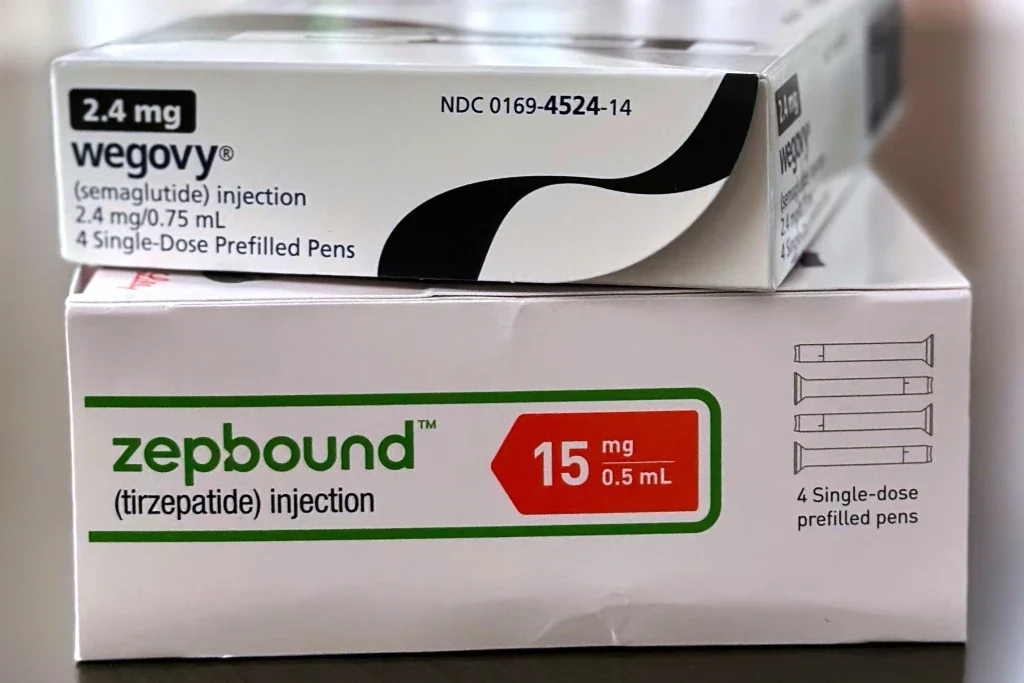
Boxes for the medications Wegovy and Zepbound are arranged for a photograph in California, May 8, 2025. (AP Photo/JoNel Aleccia, File)
It is precisely this fragmentation of authority that is now being absorbed into technological systems. The U.S. Food and Drug Administration is expanding its use of artificial intelligence to screen imported goods, relying on large-scale datasets and “quantitative analytical techniques” to identify potential risks before products reach the border. This reflects a broader shift toward a data-driven, risk-based approach to oversight.
These systems are designed to improve efficiency, but they also reshape how decisions are made. AI is now used in regulatory decision-making, with models that make predictions or decisions that influence outcomes across the drug lifecycle. Rather than relying on physical inspection to verify compliance, regulators increasingly rely on statistical inference.
This transition changes the logic of the border itself. Entry is no longer determined solely by whether a product meets a visible standard, but by how it is classified within a predictive system. In practice, the border functions as an algorithmic filter, determining which goods are allowed to circulate and which are excluded based on probabilistic assessments.
Since these systems rely on complex data and AI-driven models, it becomes difficult to trace or contest the decisions about exclusion. What is not captured within these datasets, or recognized within these models, can disappear from view. In this way, exclusion is not only enforced but produced through the system itself.
The result is a growing tension between a manufacturing landscape that is expanding supply, and a regulatory system that is refining control. On the one hand, countries like India are positioned to “rapidly expand access” to treatments, such as semaglutide, across global markets. On the other hand, importing countries are developing increasingly sophisticated systems to filter those flows using predictive classification.
This tension unfolds against a backdrop of persistent global inequality. Two billion people still lack access to essential medicines, a gap shaped by underfunded health systems, weak manufacturing capacity, and “discriminatory policies” embedded within global supply chains. International intellectual property regimes and trade agreements continue to limit countries’ ability to provide affordable care at scale.
In this context, the expansion of semaglutide exposes a deeper structural contradiction: even as production capacity grows and treatments become easier to manufacture, access remains uneven due to regulatory, economic, and political constraints. As the UN Human Rights Office emphasizes, access to medicine should be treated as a global public good, yet current governance systems increasingly prioritize managing national risk through technological control.
As semaglutide moves from scarcity to scale, the systems that govern its circulation are moving in the opposite direction. Innovation is expanding access, regulation is narrowing it. When science, behavior, and governance stop aligning, access depends less on what can be produced than on what is allowed to move.